Venous reflux disease, or chronic venous insufficiency, is a chronic vein condition of the legs that can cause swelling, cramps, and pain. With proper treatment, however, this condition can be effectively managed.
Anatomy of Veins in the Legs
Veins are designed to return blood to the heart from all areas of the body. In the legs and feet, muscles contract to push the blood upwards to the heart. To keep this blood flowing in the correct direction, leg veins contain one-way valves.
According to Merriam-Webster, reflux means “to cause to flow back or return.” In line with that definition, venous reflux disease is the condition in which some of the blood in the leg veins flows back towards the feet instead of towards the heart. This causes blood to “pool” or collect in the legs, which in turn can lead to various skin disorders and ulceration. The most common vein to suffer from vein reflux is the Great Saphenous vein, the longest vein in the body, which runs along the inside of the leg from the ankle to the groin.
Causes and Risk Factors of Venous Reflux
Causes and risk factors of venous reflux disease may include the following:
- Obesity or excessive weight
- Pregnancy
- Heredity
- Previous injury to the leg(s)
- Smoking
- Lack of exercise
- A blood clot in a deep or superficial veins
Signs and Symptoms of Venous Reflux
Common symptoms of venous reflux disease include:
- Stasis dermatitis (a type of skin inflammation in people with poor venous circulation)
- Leg edema (swelling)
- Leg achiness
- Varicose veins
- Skin ulcers
- Leg heaviness or tiredness
Some signs of a possible venous insufficiency may not be readily apparent. For instance, most healthy people who do not suffer from chronic venous insufficiency may experience some venous symptoms after standing for too long. On the other hand, some conditions such as restless legs syndrome (a strong urge to move your legs) may indicate a venous insufficiency. If you begin to notice bluish, bulging veins right beneath your skin’s surface, or you experience leg swelling and/or pain that goes away when you rest or go to bed, you may be experiencing the symptoms of venous reflux disease.
Diagnosis and Testing
After describing your symptoms to your physician, he will need to examine you both sitting down and standing up for a fuller picture of your present condition.
In order to obtain an accurate diagnosis for chronic venous insufficiency, your medical provider will likely perform an imaging test known as a Duplex ultrasound. It is important to obtain the results from this imaging test before your medical provider recommends any specific treatments, because, according to the Journal of Applied Radiology:
“Even though many patients present with varicose vein patterns that are very suggestive of a certain pathophysiology, the patterns of varicose veins seen on physical examination associated with different forms of venous incompetence overlap sufficiently to commonly result in errors of treatment selection.”
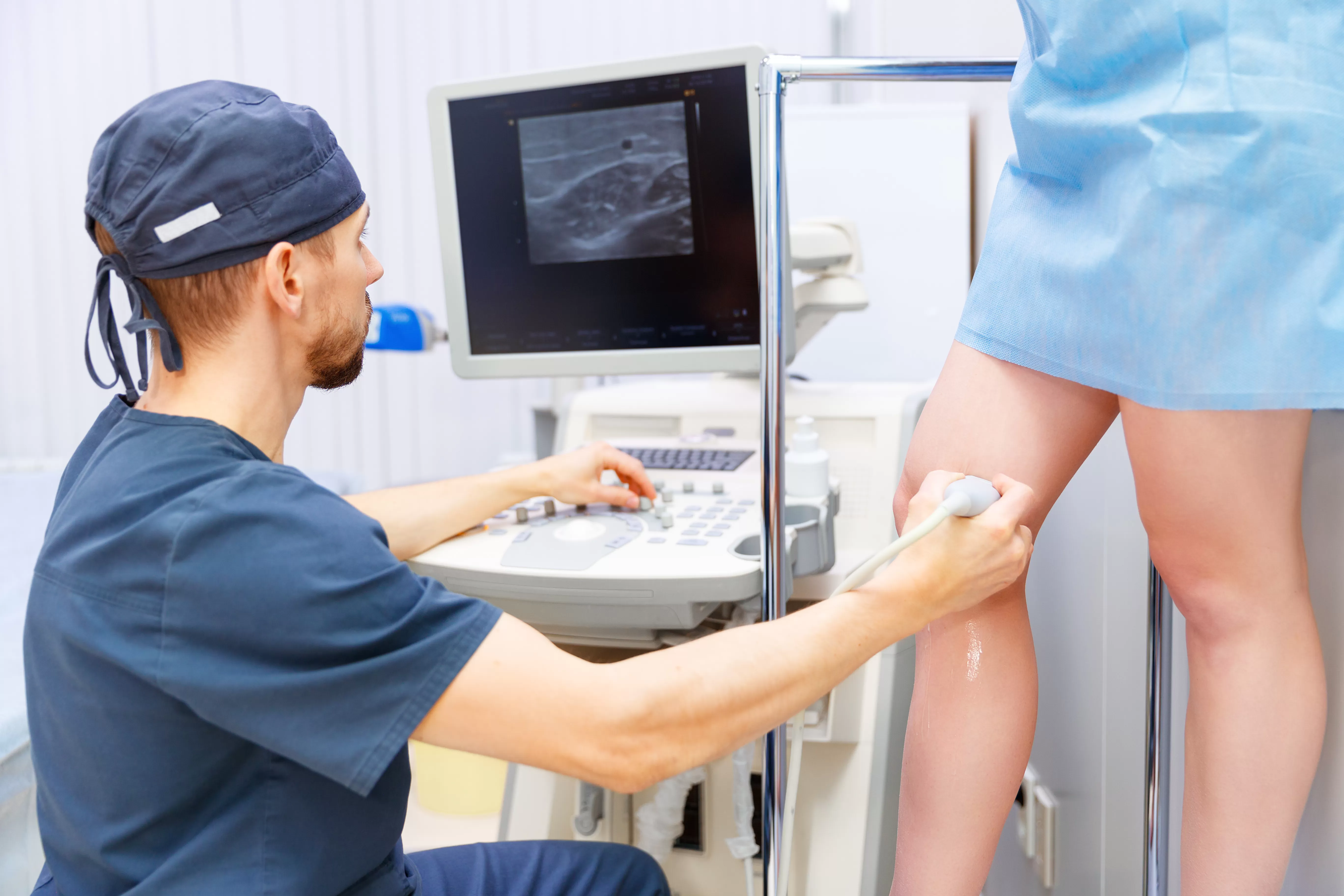
The Duplex ultrasound will examine the structure of your leg veins and the current blood flow therein. It will also check the speed and direction of your blood flow.
Venous Reflux Treatments
Once a diagnosis of venous reflux disease/chronic venous insufficiency has been obtained, your healthcare provider will craft a treatment plan based on several factors, including:
- Your age
- Your current health
- Your medical history
- The severity of your case
- Your tolerance for certain medications and/or therapies
- Your signs and symptoms
- The current prognosis
- Your personal preferences
There is a wide variety of treatment options available for those who suffer from venous reflux disease. These include the following:
Devices
There are several medical devices on the market today that are designed to mimic the body’s venous functions and serve as a compression aid to force blood upwards to the heart. Such devices, such as compression stockings, are often lightweight and can be easily hidden for maximum convenience. Usually, they do not limit mobility for the ambulatory wearer. These devices can definitely facilitate improved oxygenation and drainage; however, as these devices only provide treatment outside the affected veins without addressing the root cause, their effectiveness may be limited.
Diets
It is possible that certain lifestyle changes will effectively contribute to the treatment of your venous reflux disease. One of these changes could involve your diet. Studies have shown that the following foods and drinks should generally be limited or avoided for people who suffer from venous reflux disease:
- Red meat
- Dairy
- High-sodium foods
- Bananas
- Foods or drinks with a lot of sugar
- Alcohol
On the other hand, the following foods and drinks may help improve your condition:
- Fruits such as strawberries, mangoes, and oranges
- Vegetables such as broccoli and Brussels sprouts (it is recommended to eat fruits and vegetables raw if possible)
- Fiber-rich foods such as brown rice and popcorn
- Lots of water
Supplements
Some have recommended taking in Horse chestnut (aescin) extract to help treat venous reflux issues. This extract does contain a substance that acts as a blood thinner, so you must stop taking it before any surgical procedure. Some people have found that this supplement promotes diuresis, which in turn helps reduce fluid retention in the body’s lower extremities.
Exercise Plans
Increasing your physical activity can keep your small leg veins small, thereby reducing the amount of potential backflow. Regular exercise improves general blood circulation, which in turn can help to improve your condition. While there is no need for an unduly strenuous exercise regimen, a consistent routine of moderate physical activity can work wonders for your venous issues, and your overall health.
Endothermal Ablation
This and the next process can treat superficial venous insufficiencies. Endothermal ablation (EVLT) is a non-invasive process that involves closing down a varicose vein so that it stops working while all the adjacent veins continue functioning as normal. Only a local anesthetic is required for this procedure. Any blood that was previously used by the varicose vein would be redirected to surrounding veins. This is a relatively quick and pain-free procedure, it is also the current gold standard for vein treatment.
Sclerotherapy
Foam sclerotherapy is similar to endothermal ablation in that it targets varicose veins. Guided by ultrasound, foam is injected into the vein, thereby closing it, and causing blood flow to redirect to surrounding veins. Like ablation therapy, sclerotherapy boasts relatively fast recovery times; however, it sometimes requires multiple sessions to complete. Sclerotherapy is generally used to target the branch varicose veins near the surface of the skin. It is commonly used alongside ablation therapy.
Surgery
Surgery is the most invasive option and is generally reserved only for severe cases. The two main types of surgery for venous issues are ligation surgery and vein stripping. Ligation surgery involves tying off the vein so that it loses blood flow and eventually “dies”; vein stripping involves the complete removal of the affected vein. Both kinds of surgery have been proven effective in the treatment of venous reflux disease; however, both involve general anesthesia and the attendant risks. There is also some risk of bleeding and infection.
For a comprehensive treatment plan that addresses your particular case of venous reflux disease, be sure to consult with your attending physician or find a qualified varicose vein doctor near you.
Medically reviewed by Dr. Susanne Woloson on 5-01-2020.
*Disclaimer: We are a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for us to earn fees by linking to Amazon.com and affiliated sites.
Read This Next
Hemosiderin staining is a byproduct of the breakdown of hemoglobin and iron leaking out from veins in the legs. Hemoglobin is found in red blood cells and serves to transport...
Read MoreVenous reflux disease, or chronic venous insufficiency, is a chronic vein condition of the legs that can cause swelling, cramps, and pain. With proper treatment, however,...
Read MoreIf you notice that you have brown spots on your lower legs, feet or ankles, you may want to schedule an appointment with a vein specialist. Brown discolorations or spots...
Read More




